Pediatric Examination and Board Review (244 page)
Read Pediatric Examination and Board Review Online
Authors: Robert Daum,Jason Canel

9.
(A)
PFAPA is a benign syndrome, although frustrating to the family. The symptoms are primarily those described in the name, as well as fatigue and occasional joint or stomach pain during the fever episode. The etiology is unknown. Treatment includes antipyretics and reassurance to the parents. A recent study showed that a significant proportion of children have improvement or resolution of fever after tonsillectomy. When considering a diagnosis of PFAPA, it is important to exclude other causes of periodic fevers, including cyclic neutropenia and the known hereditary periodic fevers. Hereditary periodic fever syndromes are characterized by recurrent episodes of fever and inflammation related to inborn errors of the innate immune system, with no evidence of autoimmune dysfunction. They have Mendelian patterns of inheritance, either autosomal recessive or dominant. Gene mutations for the 4 main hereditary periodic fevers have been identified over the last 15 years. The most common of these syndromes is familial Mediterranean fever, an autosomal recessive disorder most often occurring in individuals of eastern Mediterranean origin. It usually presents during young childhood with monthly fevers lasting up to 3 days, associated with polyserositis, arthritis of lower extremity joints, myalgias, and an erysipelas-like rash. Treatment with colchicine is usually effective in preventing the fevers and the long-term complication of amyloidosis. The other hereditary periodic fevers include: hyperimmunoglobulin-D with periodic fever syndrome (HIDS), which is autosomal recessive, tumor necrosis receptor–associated periodic syndrome (TRAPS), which is autosomal dominant and often treated with the anti-TNF medication etanercept, cryopyrinopathies, which include familial cold autoinflammatory syndrome, Muckle-Wells syndrome, and neonatal onset multisystem inflammatory disease (NOMID), all of which may respond to treatment with anti-IL 1 biologics.
10.
(E)
The differential diagnosis of monoarticular arthritis is broad and influenced by several factors, including the duration and severity of joint symptoms, presence of extra-articular symptoms, and the patient’s age and gender. The differential can be divided into 5 main categories: rheumatologic, orthopedic, infectious, tumor, and miscellaneous entities. Rheumatologic diseases include oligoarticular arthritis (which involves ≤4 joints), psoriatic arthritis, juvenile ankylosing spondylitis (or enthesitis-related arthritis) and sarcoidosis, with the first 2 diagnoses more likely in this patient. Orthopedic problems affecting the knee include repetitive stress injuries, trauma, Osgood-Schlatter disease, osteochondritis desiccans, and patellofemoral syndrome, all of which, except trauma, are unlikely in a child this young. The main infectious cause to consider in a patient with a 3-month history of knee swelling is Lyme disease. Septic arthritis and osteomyelitis are unlikely in this case, considering the long duration of symptoms and the relatively mild clinical findings. Possible tumors are osteosarcoma, Ewing sarcoma, and pigmented villonodular synovitis. Although these tumors tend to occur in an older child, the clinician must always maintain a level of suspicion when the patient’s complaints are unifocal. Concern for a malignant process increases if the child has pain that is out of proportion to findings on physical examination and/or has a history of frequent focal bone pain, especially pain that awakens the child from sleep.
11.
(B)
A plain radiograph is essential in a monoarticular presentation to rule out a bone tumor. Rheumatoid factor is negative in more than 90% of patients with childhood arthritis. When present, it is usually found in older children with polyarticular disease. Furthermore, false-positive results can occur, making rheumatoid factor a very poor screening test for childhood arthritis. A joint aspiration for synovial fluid culture is not indicated in this child. The main reason to perform a joint aspiration is to rule out an acute bacterial infection, which is not expected in this case based on the long duration of relatively mild symptoms. Synovial fluid cultures aimed at recovering
Borrelia burgdorferi
are usually unsuccessful. Polymerase chain reaction of synovial fluid, and especially synovial tissue, has a much higher yield for identifying the presence of the Lymecausing spirochete. Furthermore, if Lyme disease is suspected because the patient resides in, or has traveled to a Lyme-endemic region, serologic studies (Lyme titers/Western blot) are usually performed, rather than joint aspiration.
12.
(A)
The CBC, erythrocyte sedimentation rate and CRP are often normal in oligoarticular arthritis. The ANA is positive in 40-60% of these children, usually in relatively low titer (≤1:320). It is important to recognize that the diagnosis of JIA is a clinical diagnosis, based on history and physical findings. Laboratory studies are frequently normal in multiple arthritis syndromes including oligoarticular JIA, rheumatoid factor-negative polyarticular, enthesitisrelated, and psoriatic JIA. When laboratory results are abnormal, they are often nonspecific, such as an increase in acute-phase reactants, mild anemia, or a positive ANA. The 2 notable exceptions are systemic JIA (anemia, and increased leukocyte count, platelets, erythrocyte sedimentation rate, and CRP); and rheumatoid factor positive JIA, which, by definition, has a positive rheumatoid factor and also frequently a positive anticyclic citrullinated peptide (anti-CCP), a new, more specific but less sensitive marker for this disease. Laboratory studies in children with suspected JIA may be helpful in decreasing the likelihood of other diagnoses, such as SLE, leukemia, inflammatory bowel disease, and sarcoidosis.
13.
(D)
By performing a slit lamp examination, the ophthalmologist can detect inflammatory cells in the aqueous humor of the anterior chamber of the eye. This is the best examination to detect early uveitis, an insidious eye disease in which most young patients lack eye symptoms. Later complications, such as cataracts, band keratopathy, and synechiae, can be seen by examination with an ophthalmoscope. However, by then, irreversible injury to the eye may have already taken place. High risk factors associated with chronic uveitis in childhood arthritis are female gender, young age (<6 years), positive ANA, disease duration less than 4 years, oligoarticular arthritis, and, less commonly, polyarticular (rheumatoid factor negative) arthritis and psoriatic arthritis. Children at high risk for uveitis should have a slit lamp examination every 3 months. Initial treatment for children with uveitis includes topical steroids and mydriatics. If inflammation persists, treatment with systemic CS, methotrexate, or monoclonal anti-TNF alpha medications may be indicated.
14.
(A)
The local public school district is required by Congress (Individuals with Disabilities Education Act 1975, amended in 1997, and the Disabilities Act Section 504) to provide special services to children with disabilities, including arthritis. It may not transfer this responsibility to other school districts.
15.
(E)
Although oligoarticular arthritis has a good prognosis in most patients, a significant percentage of patients may have long-term morbidity secondary to this disease. Appropriate management during periods of active disease can minimize morbidity.
16.
(D)
Isolated hip pain is extremely rare in oligoarticular arthritis. Tumor should always be included in the differential diagnosis of focal bone or joint pain. Orthopedic conditions involving the hip include Legg-Calvé-Perthes disease (idiopathic avascular necrosis) in younger children and slipped capital femoral epiphysis in adolescents. Hip arthritis occurs commonly in spondyloarthropathy. Transient or toxic synovitis of the hip is a self-limited process (usually ≤2 weeks’ duration), often noted to follow an upper respiratory infection. The child with toxic synovitis is generally 3-10 years of age, may limp, complain of pain in the hip, thigh, or knee, and may have limited hip range of motion. If there is any clinical suspicion that the patient may have septic arthritis, the hip joint must be aspirated immediately.
17.
(D)
Juvenile ankylosing spondylitis falls under the category of enthesitis-related arthritis in the JIA classification system. Enthesitis is inflammation at tendon insertion sites, for example, the Achilles insertion. Patients commonly have involvement of hip and axial joints, but they may also have arthritis of peripheral, especially lower extremity, joints. Ankylosing spondylitis is considered one of the spondyloarthropathies. The term spondyloarthropathy has historically referred to a group of entities that have certain clinical and laboratory characteristics in common: inflammation of spinal and sacroiliac joints, association with HLA-B27, absence of rheumatoid factor, occurrence of acute iritis, increased occurrence in males, and frequent positive family history of ankylosing spondylitis, inflammatory bowel disease, psoriatic arthritis, and Reiter syndrome. The presence of HLA-B27 is associated with an increased risk of developing ankylosing spondylitis, but it need not be positive to make this diagnosis. It is present in approximately 90% of whites but only 60% of African Americans with ankylosing spondylitis.
18.
(C)
The diagnosis of benign hypermobility syndrome is made by the presence of certain physical findings. These include answers B and D, as well as the ability to hyperextend the metacarpophalangeal joints when the wrist is in extension so that the fingers are parallel to the forearm, and the ability to touch the floor with the palms of the hands with the knees straight. Look for these physical findings in young children (especially between the ages of 3 and 10 years) who have increased pain after activity, as well as intermittent night pain. The incidence of benign hypermobility syndrome is increased in girls (female-to-male ratio is 2:1). It is more common in Asians and West Africans than in whites. Rarely, a small joint effusion in the ankles or knees may be observed; otherwise, there is absence of any clinical or laboratory signs of inflammation. Treatment includes parental and patient reassurance, education about this entity, avoidance of high-impact activities that increase joint symptoms, physical therapy to work on muscle strengthening, joint protection education, supportive footwear, and evening acetaminophen or ibuprofen on occasion.
19.
(D)
Growing pains, perhaps more appropriately called “benign nocturnal pain of childhood,” are characterized by lower extremity pain that frequently awakens the child (usually between ages 4 and 10 years) at night and may be associated with increased activity the day before. Laboratory and radiologic studies, if performed, are normal. Parents should be reassured. Massage may be helpful during episodes. If night awakening occurs regularly, then bedtime treatment with acetaminophen or a nonsteroidal anti-inflammatory medication, as well as a passive stretching program are helpful to decrease occurrence of symptoms. The child with this diagnosis should have no morning stiffness or other significant joint or bony pain during the day because these symptoms, in association with night awakening secondary to pain, could raise concern for an inflammatory process or malignancy.
20.
(E)
nail pitting and dactylitis
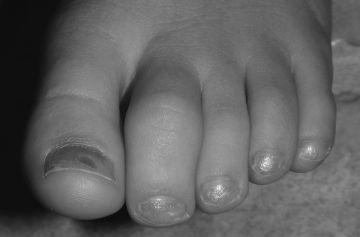
FIGURE 140-3.
Dactylitis of the 2nd and 4th toes in a patient with psoriatic arthritis.
21.
(I)
rheumatoid nodules, scleritis, and vasculitis
22.
(C)
vesiculopustular lesions on extremities and tenosynovitis
23.
(F)
erythema chronicum migrans
24.
(A)
mutation of gene encoding for pyrin
25.
(B)
conjunctivitis and urethritis
26.
(D)
resolves by 6-12 weeks
27.
(H)
erythema marginatum
28.
(G)
arthritis may precede abdominal symptoms
 S
S
UGGESTED
R
EADING