Examination Medicine: A Guide to Physician Training (8 page)
Read Examination Medicine: A Guide to Physician Training Online
Authors: Nicholas J. Talley,Simon O’connor
Tags: #Medical, #Internal Medicine, #Diagnosis

Candidates who do not want to rewrite the whole long-case presentation before facing the examiners (time is often a problem) may find it helpful to number the paragraphs with a red pen in the order in which they wish to present the story.
Many examination centres provide manila folders. These are large enough for candidates to be able to write out one whole long case on one folder. They do, however, seem to lead to a lot of turning backwards and forwards and folding and unfolding as candidates search to find where something was written. Practise with whatever method you choose so that it works smoothly.
The history-taking and physical examination
Once you have said, ‘How do you do?’ to the patient at the beginning of the long case, we suggest initially following the steps outlined below. Remember though that there is no
single right
way to conduct any part of the exam. This book is meant only to provide a framework upon which candidates can work out what suits them best. These steps may help you rapidly ascertain the patient’s major problems so that you can direct further questioning more easily.
1.
Explain to the patient that this is a very important examination. Gain the patient’s interest and support. This is a test of bedside manner.
2.
Ask the patient what is wrong. If he or she asks, ‘Am I allowed to tell you?’, look confident and firm and say, ‘Yes, of course’. Candidates are entitled to all the information the patient can offer. The examiners will usually similarly instruct the patient to tell the candidates all they can.
3.
A related but slightly different question is, ‘What do you see as the main problem with your health at the moment?’ Expect more than one problem!
4.
Ask why the patient is in hospital this time (i.e. is he or she an inpatient or outpatient?) and, if relevant, the presenting symptoms when he or she was admitted. A number of patients are brought in specifically for the examination and will have no acute medical problems.
5.
Ask early on what medications the patient is taking. A full list should be provided for you by the examination centre. This will give you valuable information about both current and past problems and is usually, but not always, helpful (
Table 4.1
).
Table 4.1
A medication list provided by a patient with extreme interest in her medical condition
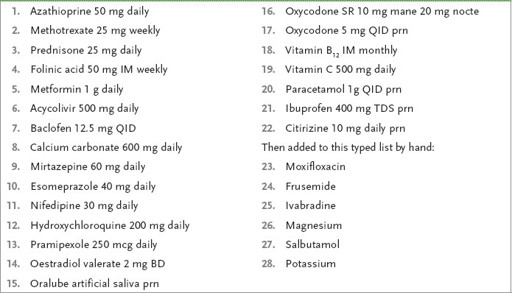
Although a list of medications is usually a big help, this one might cause anxiety for the examiners and candidates.
6.
Ask the patient about any recent tests, again to obtain clues about the current problem.
7.
If, as you probe, the patient stops talking, ask, ‘Anything else?’ and repeat as needed.
In the majority of long cases, the patient has a chronic illness about which he or she may be very well informed. It is sensible to make use of this knowledge, but remember the trap that patients may be biased in their opinions and give (inadvertently) false information. Be sceptical about patients’ opinions regarding their diagnoses and ask questions that will help verify what the patient has said. For example, a patient who says he has had five heart attacks, but has not been admitted to hospital for any of them, is probably mistaken. A candidate who merely repeats to the examiners what the patient has said without any attempt at interpretation does not come across as a sophisticated physician. Many experienced patients bring in a typed summary of their medical problems. The examiners have decided to tell patients to use these as an
aide memoire
for answering the
candidates’ questions, but not to hand them over. Candidates should exercise scepticism when patients bring in large amounts of medical information about themselves. Some patients have an exaggerated interest in their health and there have been a few suspected Munchhausen patients might slip into the exams (
Table 4.1
). It is the sign of a mature candidate that he or she can manage ‘difficult’ patients.
Having established the main diagnosis early, confirm this with specific questioning. On finding symptoms not fitting the diagnosis, decide the likely possibilities and follow up with further questions. Never blindly believe the patient.
Next, enquire about other problems. Most long-case patients are chosen because they have multiple medical problems. An example might be an elderly woman with interstitial lung disease as her major presenting illness, who also has significant ischaemic heart disease and chronic kidney disease and peptic ulceration secondary to aspirin use. It is a terrible experience to discover another major illness only minutes before the end of the time. List all the important diseases chronologically and obtain full details about each one. Organise to present the most important (i.e. often the current) problem first, followed by the others in order of importance. Some healthy scepticism about the patient’s opinion of the diagnosis is usually warranted. A history of exotic previous illnesses without a history of appropriate investigations or treatment for such conditions should prompt a careful retaking of the history.
It is important to appreciate the great amount of detail the examiners will expect about the patient’s past history. A lot of time needs to be spent on this. Failing to uncover a medical problem from long ago that the examiners found when they saw the patient counts against the candidate. Remember that the patient’s history is often well rehearsed after the examiners and perhaps another candidate have taken it.
If the patient has an illness that can become suddenly severe or life-threatening – for
example, asthma or insulin requiring diabetes – ask whether there is an
action plan
. That is, does the patient know what to do or whom to contact if he or she becomes suddenly worse? All patients should be asked about their immunisation status, including influenza, hepatitis A and B and pneumococcus.
Do not ever forget the social history. This is especially important because the examiners (and society) are keen to have caring specialists who are fully aware of the complete social environment of their patients. The examiners will expect great detail here as well. Always ask about:
•
occupation
– now and in the past
•
adequacy of income
– particularly if the patient is on a pension, can the patient afford medications and transport to appointments?
•
current housing arrangements
– e.g. renting, mortgage
•
ability to cope and resilience
at home and the quality of life if this is a chronic disease problem – the activities of daily living (ADLs) should be assessed
•
stress points
– are there problems in the patient’s life which make coping with the illness much more difficult, e.g. threatened loss of their driver’s licence
•
depression
– it is reasonable to ask patients if the illness or other problems have been associated with depression, loss of interest in life and even suicidal thoughts, but be tactful; also consider anxiety. Don’t miss post-traumatic stress disorder in a returned war veteran
•
mobility
– particularly the number of steps that need to be climbed at home and at work, and on which floor of the building the patient lives
•
hobbies
– e.g. contact with animals, chemicals or dusts
•
marital status
and number of children (from which partners)
•
sexual problems
– particularly ask about erectile dysfunction in men if indicated (e.g. patients with diabetes)
•
end-of-life decisions
– discussion of this may be appropriate if the patient has an incurable disease
•
place of birth
•
overseas travel
in relationship to the illness.
A family history must also be taken. This sort of information is easy to obtain and fills in discussion time neatly, but disaster can threaten if the candidate does not know it. The most important aspects should be outlined in your initial presentation and the rest kept in reserve to be unleashed if the examiners show an interest.
There has been recent debate about the need for candidates to take a detailed sexual history. In reality this is only necessary if it is related directly to the patient’s medical problems, e.g. someone with HIV infection. It would not be usual for a doctor to take this type of history during a first consultation, except in these circumstances. If asked why you had not taken a more detailed sexual history a reasonable answer would be that it was not directly relevant and that your usual practice is to wait until you know the patient better before asking questions of this sort.
As you examine the patient, always ask when the examiners came, what parts they examined and whether any comments were made about the signs. One candidate was told by his patient that during a fundoscopic examination the examiner had said: ‘What an interesting Roth’s spot!’ However, this is no substitute for a thorough examination.
Even though you should spend most time on the relevant systems, remember that sometimes unexpected signs will crop up, such as a large breast mass, gross papilloedema or an abdominal mass. The examiners always have in front of them a list of the signs and have always gone to the trouble of checking that, in fact, these signs are present. You
will be expected to have found all the important signs, so be thorough. Any equivocal findings should probably be ignored. Ask the proctor attendant for the results of the urinalysis and rectal examination; you are not expected to perform these personally. Also, don’t forget to take the patient’s blood pressure at some stage and check for a postural change, if at all relevant (e.g. diabetes mellitus).
Practise performing quick screening tests e.g. GALS (gait, arms, legs and spine (Ch 9) as a test of mobility, and have an approach to assessing diabetic patients for their possible vascular and neurological complications quickly.
At the end of the history-taking and physical examination, always ask the patient: ‘Is there anything else you think I should know?’ Amazingly important information is often volunteered at this point. Then ask yourself: ‘Could this be anything else?’, and ‘Can I tie all the multisystem problems into one disease?’ (usually you can’t in an older person, but this may be possible in a younger patient).
During the 20 minutes or so remaining, decide what type of case it is – that is, is it a
treatment
problem or a
diagnostic
problem, or both? Sort out the active from the inactive problems. Draft your introductory statement; for example, ‘I saw Mrs J Smith, a 30-year-old woman, who presents for the treatment problem of active rheumatoid arthritis and also for the diagnostic problem of jaundice’.
Next, mentally rehearse presenting the history and examination concisely and clearly. There is a tension between detail and brevity in the presentation of the patient. Experience and practice will help you get this right. Your concluding statement should reiterate the problems (in order of importance). It is usual to end the presentation by requests for relevant investigations. Always formulate a differential diagnosis, even if the history and examination lead to a definite diagnosis. Create a list of the findings on history and examination that support (or refute) the diagnoses considered. If a positive diagnosis cannot confidently be made, try to decide on the most likely diagnosis.
The discovery of a major problem with a particular long case (e.g. a patient with obvious dementia) shouldn’t lead to panic. By recognising the problem, fully examining the patient and having a plan of management (finding reversible causes, eliciting from relatives the social set-up, etc.), you will pass. One candidate who was faced with a demented patient in the long-case examination became angry and complained bitterly to his examiners. He failed.
Occasionally there are other difficulties, such as language problems (usually the candidate is supplied with an interpreter) or the patient becomes ill during the time (cardiac arrests have occurred). Be sure to inform the proctor attendant of any difficulties; people will go out of their way to be fair in such circumstances. The examiners will make a note of any such problems on their scoresheet, so that this can be taken into account by the executive later on. As the first question, the lead examiner will ask the candidate if there were any problems with the patient during the case. This is not the time to complain about the patient. The examiner will know if the patient was a difficult historian. However, if there were problems, such as late arrival of the patient or the patient’s need to leave the room a number of times to go to the toilet, this should be mentioned, but not dwelt upon.
The presentation
Your whole presentation to the examiners should take 10–12 minutes. Never go longer, ever! Leave out any irrelevant detail; padding the presentation never impresses. Avoid repetition; for example, mentioning various medications as a part of the history of a
particular system and then later as part of a long general list. Try not to use the brand names of drugs.